
Professor
MD, PhD, Both at University of Crete School of Medicine
Specialty: Vascular Surgery
Major Interest: Myopathy of Peripheral Arterial Disease
The laboratory of Dr. Pipinos and his partner Dr. Casale is a highly interdisciplinary environment. The major focus of the laboratory is the development of regenerative medicine strategies for skeletal muscle tissue in the legs of patients suffering from peripheral arterial disease (PAD). PAD afflicts 5% of the US population older than 55 years of age and develops along with hardening (atherosclerosis) of the arteries of the legs. PAD is a chronic condition that decreases the blood supply to the legs producing significant damage to the muscle. Patients with PAD limp and can only walk very short distances because the muscle in their legs is damaged and their legs hurt. Our laboratory evaluates the mechanisms that produce the leg dysfunction of claudication and our work aims to ultimately improve patient prognosis and produce significant new diagnostic and treatment strategies for the care of claudicating patients. Our research group is involved in multiple projects and involve the combined efforts of biomechanists, life scientists, biomedical engineers, physicians, veterinarians, and a strong technical support staff.
Our principal research interests include:
- Regeneration of adult skeletal muscle with the use of exercise, medications, adult stem cells, exoskeletons and revascularization operations
- Mitochondrial dysfunction, oxidative damage, fibrosis and inflammation in the leg muscle of patients with PAD
- Atrophy in the leg muscle of patients with PAD with special focus on myofiber degeneration and muscle fibrosis
- Biomechanical analysis of the gait of PAD patients
- Developmental Biology and its role in Regenerative Medicine
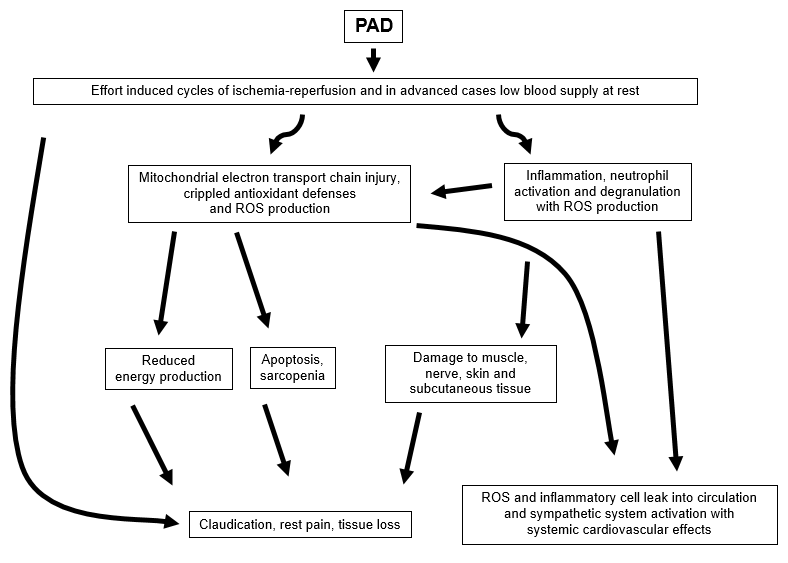
Proposed pathway for the pathogenesis of PAD manifestations. The fundamental problem in PAD is obviously the presence of arterial occlusive disease. Arterial stenoses and occlusions produce effort-induced cycles of ischemia and reperfusion. These cycles initiate a combination of oxidative stress and inflammation, which sets in motion a cascade of injury to muscle cells and their organelles along with cellular apoptosis and necrosis. Key players in the chronic phase of this process are dysfunctional mitochondria that, through multilevel failure in their roles as energy, oxygen radical species, and apoptosis regulators, produce and sustain a myopathy with progressive decline in muscle performance. This myopathy is the better explored component of this process in PAD limbs, and its nature is the main focus of the present review. However, there is increasing evidence demonstrating that the injury route expands to involve every structure in the leg including nerves, skin, and subcutaneous tissues. Claudication, rest pain, and tissue loss then emerge as the external manifestations of ongoing tissue functional deterioration and injury. PAD indicates peripheral arterial occlusive disease; ETC, electron transport chain.

