Like many young children, Hudson Campbell had plenty of ear infections in the first few years of his life.
He got his first set of ear tubes in 2019 when he was about 2 years old. At the time, his family was living in Louisiana, where his father, Maj. Gregg Campbell, was stationed with the U.S. Air Force.

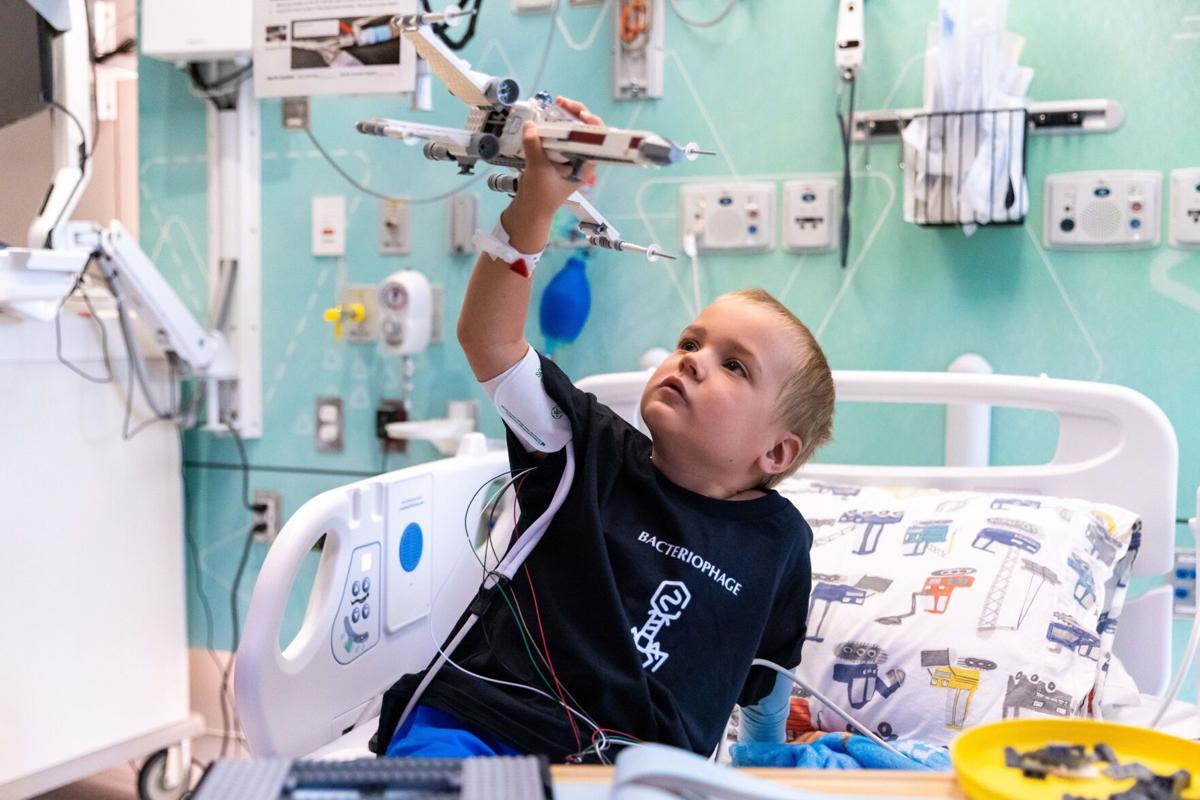
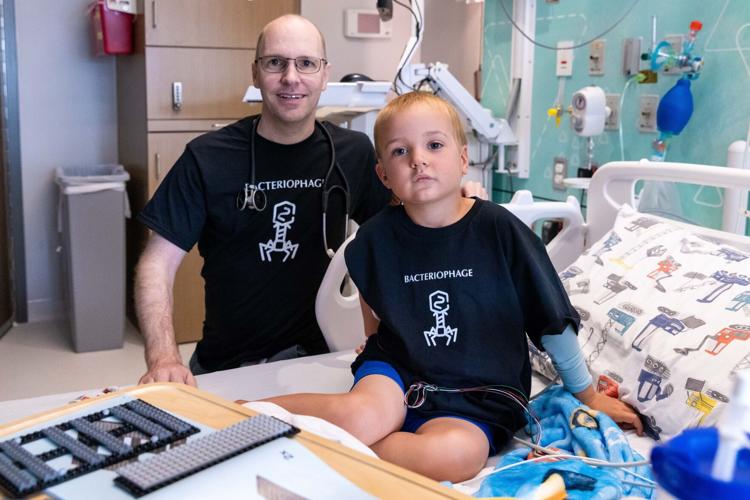
Hudson Campbell, left, plays with Legos with dad Gregg Campbell at Children’s Hospital & Medical Center. Hudson’s doctor is using a virus called a bacteriophage to target a bacteria in his left ear that is resistant to many antibiotics.
But after more infections, several different antibiotics and two additional sets of tubes — the last after his family moved to Omaha in June 2020 — a bacterial culture collected by a local ear, nose and throat physician revealed that Hudson had no ordinary infection. Instead, it involved a type of bacteria called Mycobacterium abscessus. While infections with the bacteria are relatively rare, Mycobacterium abscessus is known for being resistant to many antibiotics.
As a result, Hudson has required no ordinary treatment. The youngster, who just turned 6, has been on long-term antibiotic therapy for much of the past two and a half years, including several newer antibiotics used for the first time at Children’s Hospital & Medical Center. He’s faced a host of side effects and setbacks, including allergic reactions to some drugs and the loss of most of his hearing.
People are also reading…
Now in addition to an antibiotic cocktail, Hudson recently started receiving a longtime adversary of bacteria: a type of virus called a bacteriophage. His bacteriophage, or phage for short, was selected specifically to match his strain of the problem bacteria.

Dr. Bradford Becken gave Hudson Campbell a plush bacteriophage like the real version that Becken is using to try to clear a bacteria that is resistant to many antibiotics.
Dr. Bradford Becken III, a pediatric infectious diseases physician at Children’s, said his hope is that the phage therapy — a first for Children’s — will help clear lingering infection in Hudson’s left ear that appears to be clinging to a wire placed in February 2022 to support a cochlear implant, which failed.
Normally, Becken said, doctors would remove the wire. But then a crucial nerve could atrophy, making it nearly impossible to place a new implant and restore hearing on Hudson’s left side. Hudson has a cochlear implant in his right ear, which has been cleared of infection.
Hudson is receiving the phage therapy intravenously and, in what is believed to be a first in the U.S., via drops placed directly in his ear twice a day. A PET scan in July is expected to determine whether any infection remains and whether the wire can stay or will have to go.
“Our thought is, ‘If we also put the phage in his ear, maybe that will give him a better chance of clearing this infection without having to have that wire removed,’” said Becken, an assistant professor of pediatric infectious diseases at the University of Nebraska Medical Center who began seeing Hudson in late 2020.
Phages kill bacteria — they don’t infect people — by injecting their DNA into bacterial cells and using them to make more phages. Discovered about 100 years ago, phages have been more commonly used therapeutically in parts of Eastern Europe. They’re found naturally in places ranging from soil to the human gut.
The West, on the other hand, has largely relied on antibiotics to treat microbial infections. But with the rise of microbial resistance to those drugs, Becken said, phages are having a moment.
More than 2.8 million antimicrobial-resistant infections occur in the U.S. each year, with more than 35,000 people dying as a result, according to the Centers for Disease Control and Prevention’s 2019 Antibiotic Resistance Threats Report. Worldwide, an estimated 1.7 million deaths were directly attributed to resistant infections in 2019 and nearly 5 million deaths were associated with bacterial resistance, according to a report in The Lancet.
Becken said he would like to see phages become more commonly available for use in cases where clinicians have to rely on broad-spectrum antibiotics for hard-to-treat infections like Hudson’s that require months of therapy. He estimated that phage therapy is used somewhere between 50 and 100 times a year for infections of all types.
He also would like to see new technology that would allow for faster identification of infections where phages might be useful, as well as those that would expedite the process of finding the right phage for an infection. Currently, molecular testing allows clinicians to quickly screen samples for common bacteria and to check for common genes that convey antibiotic resistance.
Kylie Campbell, Hudson’s mother, also would like to see greater awareness and a more streamlined system. The process of testing and getting legal approval for Hudson’s therapy, including obtaining a green light from the Food and Drug Administration, “took way longer than as a mother I would have expected,” she said.
She said she understands the caution, however, given the newness of the therapy. But she sees phages as good option because they’re specific to a patient’s bacteria and are associated with few side effects.

Dr. Bradford Becken, left, a pediatric infectious diseases physician at Children’s Hospital & Medical Center, has called on a longtime adversary — a type of virus called a bacteriophage — to treat an antibiotic resistant bacteria in Hudson Campbell’s ear.
“What we forget is we have terrific medications in the world right now,” said Campbell, a physical therapist. “But there are so many side effects, especially when you’re having to be on long-term use of anything.”
Hudson’s phage — identified on a third round of screening — came from the lab of Graham Hatfull, a microbiologist and professor of biotechnology at the University of Pittsburgh.
Hatfull and his team published a paper in Nature Medicine in 2019 about their use of an engineered phage cocktail to help treat a young cystic fibrosis patient who developed a life-threatening Mycobacterium abscessus infection after a double lung transplant. (Hudson, on the other hand, is an otherwise healthy child, Becken said, with no other underlying health conditions. How the youngster acquired Mycobacterium abscessus isn’t known. It exists in water and soil, particularly in warm, humid environments, and has been known to contaminate medical devices.)
Hatfull said his lab has received about 380 requests to find phage matches for the bacteria since that time. His lab, the university and a program called SEA-PHAGES, or Science Education Alliance-Phage Hunters Advancing Genomics and Evolutionary Science, have archived more than 22,000 phages. The program tasks undergraduate students with finding phages in soil and identifying them in a lab. Hatfull serves as lead scientist for the program, which he and his team administer with the Howard Hughes Medical Institute’s Science Education Division.
In some cases, he said, a doctor has been treating the infection for a year or two — or more — and has run out of options.
“I wouldn’t make any claim by any means that phages are a universal solution or a panacea,” Hatfull said, “but I think that they provide a potential alternative option when the physicians have run out of all others.”
Hatfull said it’s not uncommon for the lab to receive multiple samples of bacteria from a patient to screen. Sometimes, the pathogens in a patient change over time. Clinicians may not get all representatives of a bacterial mix when they sample.
But he said the therapeutic use of phages appears safe and correlates with favorable clinical outcomes in some patients.
“We’re not really looking for miracle cures but ... to see if we can tilt the balance in the favor of the patient ... and to do it in a way that the risks to the patient are pretty minimal,” Hatfull said.
It remains to be seen whether the use of phages takes off, he said. One impediment is the fact that the researchers don’t have enough phages to find a good match for about half the strains they get. Some of that may be addressed by finding more phages, developing phage cocktails and using genetic manipulation.
Hudson already has been through a lot of treatments. Becken said he began treating him with a mix of intravenous and oral medications after Hudson was referred to him. It took about a month to find the right regimen. Hudson continued on that for about six months. Hudson had no outward signs of infection after that, so the team stopped treatment.
But within about two weeks, Becken and Campbell recalled, the infection came back — worse than before.
In July 2021, Campbell said, Hudson woke up one morning essentially deaf in both ears.
Becken said Hudson’s hearing loss likely was due to a combination of the infection and one of the drugs he was taking, which is known to be toxic to the ears, with the infection likely playing the larger role. The drug, however, was one of the best available for treating his condition.
Campbell noted that opting to use it was one of the many risk-vs.-benefit decisions the family and Hudson’s caregivers have made during his treatment.
Hudson started a new regimen in August 2021. A CT scan, however, indicated infection in the mastoid bone behind his ear, she said. Hudson underwent surgery at the Mayo Clinic that fall.
Later that year, the family and Hudson’s caregivers also weighed how to keep Hudson hearing and still treat his infection. He wanted to hear his parents’ voices again, Campbell said. Hearing aids hadn’t worked because of all the drainage in his ears and because his hearing loss was so profound.
Hudson initially got a cochlear implant on the left side in February 2022. But within a month and a half, the incision opened, exposing the implant. Hudson returned to the Mayo Clinic for a second surgery to clear out the ear canal. Surgeons also placed a cochlear implant on the right side, which had been clear of infection for about six months.
“He’s done terrific with the cochlear implant,” she said.
Meanwhile, Becken had been consulting with experts across the country, including teams at the Veterans Administration and Case Western Reserve University who were working with novel drugs and drug combinations. Hudson started some, one of which required a novel drug application and approval from the FDA. The family traveled to the National Institutes of Health in Washington, D.C., last summer to visit an expert on his bacteria, with whom Becken also had been corresponding.
Becken also continued to explore phage therapy. Campbell said a culture last August — the bacteria takes up to 90 days to grow, testing an additional month — resulted in a match that led to the start of his phage therapy late last month.
Becken said Hudson has been tolerating the phage well. Now his goal, and that of Hudson’s family, is for the youngster to have as normal a childhood as possible and for the infection to fade to a memory.
Campbell said Hudson successfully completed kindergarten and will move on to first grade this fall. He plays tennis and his favorite activity is swimming.
Because of that, she was determined last summer to figure out how to make Hudson watertight for the pool, a process that takes about 30 minutes. He wears a custom ear mold in his left ear and a water box on his cochlear implant that allows him to hear in the water. A waterproof sleeve secured with waterproof tape covers the long-term IV access point in his arm for his medications.
“There’s no prize for being the first person to put ear drops in someone’s ear,” Becken said. “Let’s just get the patient better and give other patients in the future more options.”
Our best Omaha staff photos & videos of June 2023

LSU's Nic Bronzini (14) and Christian Little (99) celebrate following the Florida vs. LSU, game three of the College World Series championship series, in Omaha on Monday. LSU won the title 18-4.

Florida's Brandon Neely (22), from left, Tyler Shelnut (6) and BT Riopelle (15) give autographs to young fans following the Florida vs. LSU, game two of the College World Series championship series, at Charles Schwab Field in Omaha on Sunday, June 25, 2023. Florida won 24-4.

LSU's Tommy White (47) celebrates his walk-off homer in the Wake Forest vs. LSU CWS men's College World Series, game thirteen in Omaha on Thursday. LSU won in a walk-off home in the 11th inning.

LSU's Gavin Guidry (1) throws a ball against the wall of the bullpen in the Wake Forest vs. LSU CWS men's College World Series, game twelve in Omaha on Wednesday.

Ivie Galvan, right, of Goodyear, Ariz., and her aunt Sarah Shortbull, of Yankton, S.D., sit in the stands ahead of the Florida vs. TCU CWS men's College World Series, game eleven in Omaha on Wednesday.

Tennessee's Maui Ahuna, left, talks to the first base coach in the third inning against LSU during game nine of the College World Series on Tuesday, June 20, 2023.

Drone photography of J & S Feedlot and Farm, with about 2,000 head of cattle, near Dodge, Neb., on Tuesday. With Dodge County under extreme or exceptional drought, owners Joan and Steve Ruskamp have had to adjust how they care for their cattle.

A Tesla coil electrifies a baseball in the World-Herald on Wednesday.

An Omaha police officer keeps people away from where a suspicious package that prompted a law enforcement response near gate 2 at Charles Schwab Field on Thursday, June 15, 2023.

An Omaha police officer carries a suspicious package that was found near gate 2 at Charles Schwab Field on Thursday, June 15, 2023.

Florida's Josh Rivera shows off his glove after practice on Thursday, June 15, 2023.

TCU's Tre Richardson stretches before practices on Thursday.

Lt. Dennis Svoboda, with the Sarpy County Sheriff's Office, leads a training session on an airboat for the search and rescue team on the Platte River near Louisville, Neb., on Thursday, May 25, 2023.

Sculptor John Lajba walks about his Road to Omaha Sculpture before cleaning it at Charles Schwab Field on Wednesday, June 07, 2023.The sculpture was dedicated exactly 24 years earlier at Rosenblatt Stadium.

John Lajba scrubs his Road to Omaha Sculpture at Charles Schwab Field on Wednesday.

John Lajba spray washes his Road to Omaha Sculpture at Charles Schwab Field on Wednesday.

Kaitlyn Emanuel, a North Bend Central three-sport athlete, is the Omaha World-Herald girls Athlete of the Year. Photographed at her family's farm outside North Bend, Neb., on Friday.

2023 All-Nebraska baseball team captains Millard South's Cam Kozeal, left, and Omaha Gross's Connor Capece pose for a portrait on Thursday.

Police closed Hamilton Street near 30th to investigate a shooting early on Wednesday.

A dog peeks out of a window and watches as police investigate a shooting near 30th and Hamilton Streets on Wednesday.

Omaha police and forensics investigators look for evidence as they investigate a shooting that injured one person near 30th and Hamilton Streets on Wednesday.

Omaha police investigate a shooting that injured one person near 30th and Hamilton Streets on Wednesday.

Some of the leather bags from Jared Hall's 3am Luxury brand.

The Omaha fire department investigate the scene after a forklift struck a propane tank and caused an explosion at 4301 N 30th St. a on Monday. One person was seriously injured.

A woman is visible distraught after a forklift struck a propane tank and caused an explosion and blew the garage doors off of a building owned by Omaha Public Schools located at 4301 N 30th St. a on Monday. One person was seriously injured.

O.NE Finest dancers perform during a hometown send-off for Terence “Bud” Crawford ahead of his fight with fellow welterweight world champion Errol Spence on July 29. Photographed at B&B Sports Academy in North Omaha on Saturday.

Julia McGuigan, facing, demonstrates a drawing technique with student Anahi Salazar during an "Urban Illustration" workshop at her studio and shop north of downtown Omaha on May 12.