Mohs Micrographic Surgery, Reconstruction
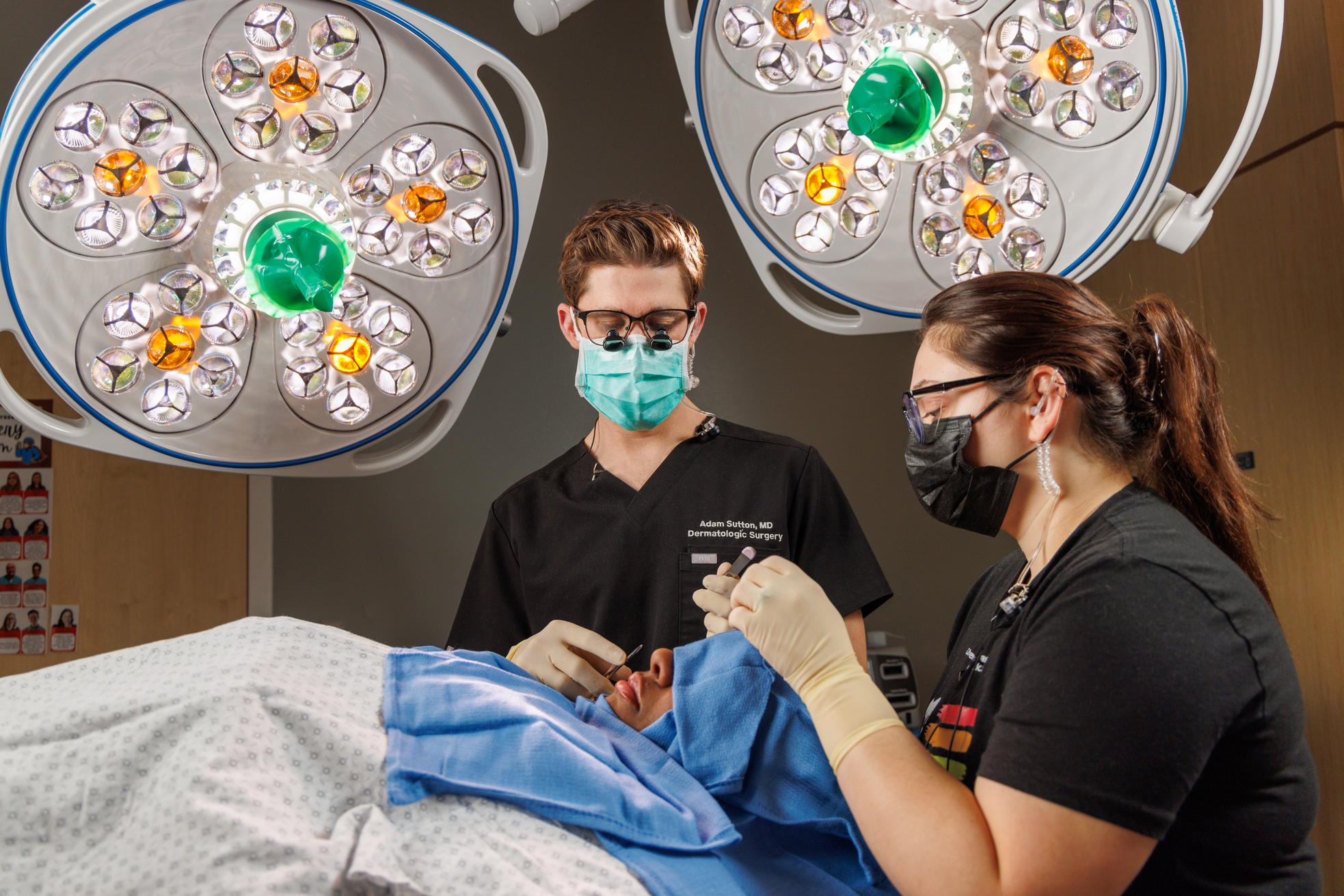
Dermatology trainees at UNMC learn from fellowship-trained surgeons on the highly specialized Mohs procedure.
The Mohs procedure was named for its inventor, Frederic Mohs, MD. UNMC faculty members Adam Sutton, MD and Vanessa Voss, MD are "grandchildren" of Dr. Mohs, having trained with Hubert Greenway, Jr., MD, who trained directly with Dr. Mohs.
Dr. Sutton serves in national leadership roles in the American College of Mohs Surgery, which was founded by Dr. Mohs.
Learn more about Mohs Micrographic Surgery at Nebraska Medicine.