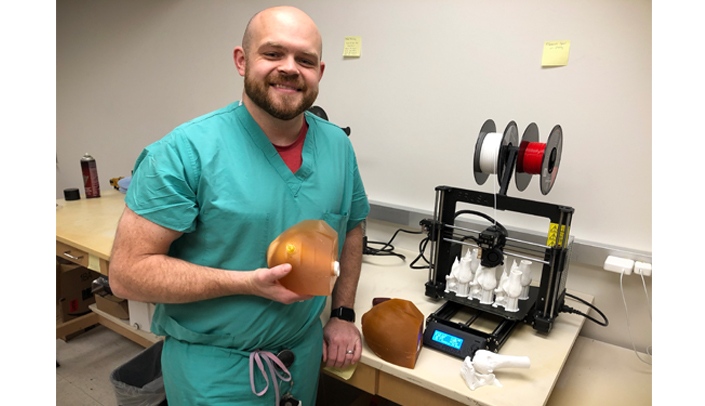
Nick Markin, M.D., director of perioperative imaging, was awarded a $5,000 Educational Support Grant from the College of Medicine for an ongoing project that utilities 3D printing to create educational simulation models.
The simulation models will assist physicians in sharpening their intraosseous infusion skills. To perform an intraosseous infusion, a provider drills through the shoulder tissues and humerus bone to inject vital fluids directly into the marrow. This technique provides a non-collapsible entry point, and is utilized when intravenous access is not feasible. Performing an intraosseous infusion is rare, but can be vital in emergency scenarios.
"The presence of a simulation model and a regimen to practice intraosseous infusions can increase physician competence to utilize this procedure, which could save lives in high-stake scenarios," said Dr. Markin.
Dr. Markin has explored the idea of custom-making simulation models to meet his educational needs for the past five years. His implementation of 3D printers in 2018 kicked his projects into high gear, and allows him to make highly-customized models.
Creation of an intraosseous infusion model begins by printing a portion of the humerus bone with a hollow cavity in place of marrow. That simulated bone portion fits inside a custom-made mold. A specialized gelatin is poured in and left to cool. When the mold is removed, the gelatin has become solid and resembles a portion of the human shoulder, complete with a hidden model humerus bone inside. When gelatin has depreciated from use, it can be removed, melted down and molded again.
A section of six humerus bones takes more than 30 hours to complete using a 3D printer. However, what’s lost in promptness is gained in frugality. These homegrown intraosseous simulators cost handfuls of dollars and can be tailored to fit unique educational needs, while mass-produced simulators cost hundreds with recurring replacement part expenses. The grant funds will help cover the cost of equipment and materials.
Once the simulation models are complete, Dr. Markin will study their effectiveness in translating skills from practice to reality. He has enlisted the help of a researchers Alicia Schiller, PhD, and Martina Clarke, PhD, who execute translational and qualitative research, respectively. The team will test physicians before and after the use of the simulation model to analyze their confidence and competence with intraosseous infusions. They will also test the resilience of confidence and skill levels over time with the goal of reintroducing trainings before regression of skills.
"The whole idea with this project is that we want people to have regular access to educational tools that allow them to transfer their competency to real-life scenarios that enhances patient care," said Dr. Markin.
Dr. Markin Awarded $5,000 for Homegrown Simulation Models
- Written by Danielle Beebe
- Published May 13, 2019